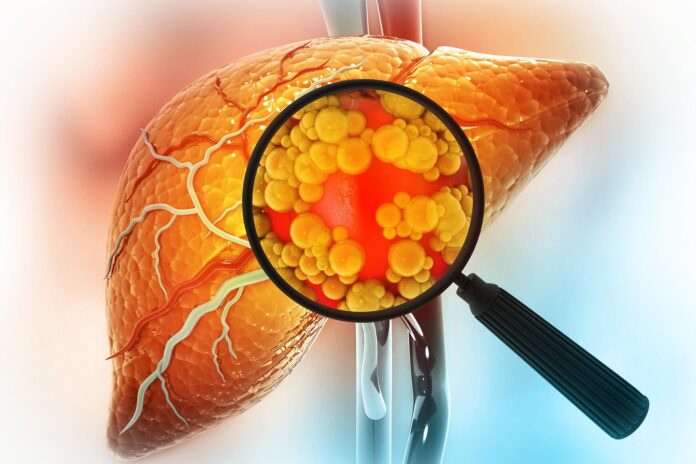
Researchers at the Johns Hopkins Kimmel Cancer Center have developed an artificial intelligence-powered blood test capable of detecting silent liver disease long before clinical symptoms emerge. This innovative approach analyzes the structural patterns of DNA fragments circulating in the bloodstream, offering a non-invasive method to identify early-stage fibrosis and cirrhosis.
The study, published in Science Translational Medicine and supported by the National Institutes of Health, marks the first large-scale application of “fragmentome” technology—a method previously reserved for cancer research—for diagnosing chronic, non-cancerous conditions. By leveraging machine learning to interpret genome-wide DNA fragmentation, the team has created a tool that could transform early intervention strategies for millions of patients.
How the Fragmentome Reveals Hidden Disease
Traditional liquid biopsies typically search for specific genetic mutations associated with cancer. In contrast, this new technology examines the fragmentome : the physical characteristics of cell-free DNA (cfDNA) fragments, including their size and distribution across the genome.
When cells die, they release DNA into the bloodstream. The way this DNA is fragmented reflects the physiological state of the body. While cancer research has focused on finding mutated sequences, Johns Hopkins scientists discovered that the pattern of fragmentation itself contains critical health data.
For this study, the research team analyzed whole-genome sequencing data from 1,576 individuals, including those with liver disease and other health conditions. They evaluated approximately 40 million DNA fragments per sample across thousands of genomic locations, incorporating repetitive DNA regions that had previously been overlooked. Machine learning algorithms processed this massive dataset to identify specific fragmentation signatures linked to liver damage.
“The fact that we are not looking for individual mutations is what makes this study so powerful,” says Akshaya Annapragada, M.D./Ph.D. student and first author of the study. “We are analyzing the entire fragmentome, which contains a tremendous amount of information about a person’s physiologic state.”
Why Early Detection Matters
Liver disease is often asymptomatic until it reaches advanced stages, making early detection crucial. According to Dr. Victor Velculescu, co-director of the cancer genetics and epigenetics program at Johns Hopkins and co-senior author of the study, an estimated 100 million people in the United States have liver conditions that increase their risk for cirrhosis and liver cancer.
Current diagnostic methods have significant limitations:
* Standard blood tests often fail to detect early fibrosis.
* Cirrhosis detection via existing methods is accurate only about half the time.
* Imaging technologies, such specialized ultrasound or MRI, are not always widely available or accessible.
Liver fibrosis is reversible in its early stages. However, if left undetected, it can progress to cirrhosis, significantly increasing the risk of liver cancer. The new AI classifier demonstrated high sensitivity in detecting early liver disease, advanced fibrosis, and cirrhosis, potentially allowing doctors to intervene before irreversible damage occurs.
From Cancer Research to Chronic Disease
The project originated from a 2023 study on liver cancer fragmentomes published in Cancer Discovery. While reviewing data, researchers noticed that patients with fibrosis or cirrhosis exhibited subtle but distinct DNA fragmentation patterns, even when their profiles appeared largely normal by conventional standards. This observation prompted the team to investigate whether these patterns could serve as reliable biomarkers for chronic liver disease.
Beyond liver health, the study explored the broader applicability of fragmentome analysis. The researchers developed a fragmentation comorbidity index using data from 570 people with suspected serious illnesses. This index successfully differentiated between individuals with high and low Charlson Comorbidity Index scores—a standard measure of how additional health conditions impact mortality risk. The fragmentome-based index independently predicted overall survival and, in some cases, outperformed traditional inflammatory markers.
A Platform for Multiple Diseases
The technology’s potential extends beyond hepatology. The study identified fragmentome signals associated with cardiovascular, inflammatory, and neurodegenerative conditions in high-risk individuals. Although the study did not include enough patients to build separate classifiers for each of these diseases, the findings suggest that the fragmentome platform could eventually support disease-specific tests for a wide range of chronic conditions.
“A liver fibrosis classifier is distinct from a cancer classifier,” explains Annapragada. “This is a unique, disease-specific test built from the same underlying platform. These classifiers are disease-specific and do not cross-react.”
Next Steps and Clinical Availability
Despite these promising results, the liver fibrosis assay described in the study remains a prototype and is not yet available for clinical use. The research team emphasizes that the next phase involves rigorous validation and refinement of the liver disease classifier. Future work will also focus on expanding the dataset to develop robust classifiers for other chronic conditions identified in the initial screening.
“For many of these illnesses, early detection could make a profound difference,” says Velculescu. “If we can intervene earlier — before fibrosis progresses to cirrhosis or cancer — the impact could be substantial.”
The development of this AI-driven diagnostic tool represents a significant shift in how chronic diseases are monitored, moving from reactive treatment to proactive, precision-based prevention. By decoding the hidden signals in our DNA, this technology offers a clearer path to early intervention and improved patient outcomes.